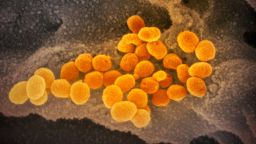
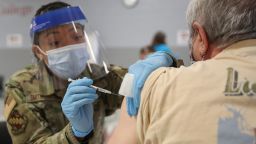
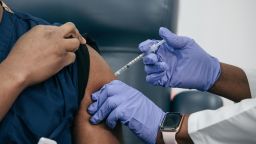
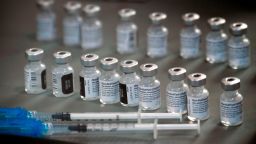
There is some encouraging news in the fight against Covid-19 as more vaccines are being distributed and several states announced they will ease certain coronavirus restrictions amid decreasing case levels and hospitalizations, but despite the promising developments experts insist Americans need to remain cautious, especially with the arrival of differing variants in the United States.
On Thursday, Stefan Pryor, Rhode Island’s Secretary of Commerce, said that starting Friday indoor dining will be allowed at 50% capacity. Catered events, he added, will allow up to 30 people indoors and 50 people outdoors with testing.
In Massachusetts, Gov. Charlie Baker said that starting Monday all businesses limited to operating within 25% capacity can raise that threshold to 40%, including restaurants.
The two states joined New Jersey, which on Wednesday announced it will ease indoor gathering limits and lift the 10 p.m. curfew for restaurants, citing decreasing Covid-19 spreading rates and hospitalization rates. Starting Friday, indoor gathering capacity limits, including for indoor dining, will be raised to 35% from 25%.
And last week, New York Gov. Andrew Cuomo announced that if the coronavirus positivity rate continued to decline – as of Jan. 29 the rate was at 4.6%, the lowest since Nov. 28 – the state could resume indoor dining at 25% capacity beginning February 14.
Additionally, 35.2 million doses of the Covid-19 vaccine have been administered in the US, according to data published Thursday by the US Centers for Disease Control and Prevention. That’s about about 61% of the 57,489,675 doses distributed, and it means about 8.5% of the US population – nearly 28 million people – have now received at least one dose of a coronavirus vaccine.
Despite the hopeful news, experts insist Americans need to remain cautious.
The emergence of these virus mutations – first detected in the United Kingdom (B.1.1.7), South Africa (B.1.351) and Brazil (P.1), respectively – could mean another surge in cases, according to Dr. Michael Osterholm, director of the Center for Infectious Disease Research and Policy at the University of Minnesota.
“What we need to do is anticipate this is coming, and I understand this is hard for the public. They’re saying give me a break, I’m tired of this. But the bottom line is we have to be prepared for what I feel is certain is coming, and that’s the challenge we have right now,” Osterholm said Thursday on CNN’s “New Day.”
It will take much more than a vaccine to “keep this variant at bay and not have potentially a major surge in just the weeks ahead,” Osterholm said, referring to the UK variant.
New variant on the rise in Florida and California
Cases of B.1.1.7 are on the rise and could become dominant in hot spots like Florida and Southern California “within a few weeks,” according to the testing company Helix, which has helped identify the largest share of variant cases in the US.
The rise of B.1.1.7 is not just a product of increased genetic sequencing across the country, Helix President Dr. James Lu told CNN late Wednesday.
More than 600 cases of this variant have been found in 33 states, according to the CDC. Most are in Florida and California. The first US case was announced December 29, but the earliest known cases stretch back at least as far as mid-December.
Researchers have said that although the B.1.1.7 variant appears to be more transmissible than previous strains, it is not known to be more deadly or cause more severe disease.
The strain has also been found in at least 80 countries and territories around the globe, the World Health Organization said this week.
“The rate of growth here in Florida and Southern California looks a lot like the type of growth that we have seen previously in the UK and Denmark … where B.1.1.7 became the predominant variant strain pretty quickly,” Lu said.
The CDC last month said modeling showed this variant could become the US’ predominant strain in March and could worsen the spread of the disease.
Rates of new coronavirus cases overall in the US have been dropping. The country has averaged about 136,900 new cases a day over the last week – the lowest average since November 12, according to Johns Hopkins University data.
But Dr. Anthony Fauci has suggested the US isn’t vaccinating people fast enough to stay ahead of new variants, and that could blunt efforts to keep bringing case levels down.
“If the variants and the mutations come, and start becoming dominant, then that’s going to obviate some of the effects of the vaccine,” Fauci, director of the National Institute of Allergy and Infectious Diseases, told CNN this week.
Fauci told CNN’s Chris Cuomo on Thursday the best way to prevent viruses from mutating and developing is to prevent them from spreading.
“And you do that by public health measures, and getting as many people vaccinated as quickly as you possibly can because viruses will not mutate if they don’t replicate,” Fauci said. “So if you put the lid on them and prevent them from going to person to person, you will blunt their capability of mutating.”
As for how Helix has tracked the B.1.1.7 variant, Lu referenced a small but growing number of samples showing a testing glitch, which signals the presence of a mutation in B.1.1.7. Not all of these samples are B.1.1.7, since the mutation can exist on its own.
There’s been an increasing rate of this glitch – known as S gene dropout – in places like Florida and Southern California. And an increasing proportion of these samples are being confirmed as B.1.1.7 once they’re genetically sequenced, Lu said.
“We’re in a race between the vaccine and the new strains,” Lu said. It’s unclear whether the pace of vaccination will prevent the strain from taking a foothold in places where it’s not already circulating, Lu added.
Helix is one of a number of commercial, academic and public health labs that share information with the CDC.
Two other strains are harder to detect, testing company says
Two other more-transmissible variants – first identified in South Africa (B.1.351) and Brazil (P.1) – have been much harder to locate, Lu told CNN Wednesday night.
That’s because the mutation that causes the “S gene dropout” glitch that helps Helix find B.1.1.7 cases is not present in the other two strains.
Beyond appearing more transmissible, the B.1.351 and P.1 strains also contain a different mutation that scientists worry could help the virus escape some of the antibody protection from vaccines or previous infection. Even so, experts say they expect vaccines will still work against the variants – especially when it comes to preventing severe disease and death.
“They’re not detectable with our level of sampling today,” Lu said of variants first identified in South Africa and Brazil. “So, most of the time, if we’re finding it, it’s serendipity right now. But that will change, if they become more prevalent.”
Last week, the first US cases of the B.1.351 strain were found in South Carolina. According to a state health official, these two cases were found during routine sequencing, but “the predominant strain that we are still seeing in our surveillance sequencing is the standard, or normal,” version of the virus. Maryland has also reported a handful of cases.
At least two cases of the P.1 strain linked to Brazil have been found in the US. Both patients live in the same household in Minnesota, and one had recently traveled to Brazil, according to the state’s health department.
Coronavirus deaths in US
Though daily case levels and the number of coronavirus patients in hospitals are dropping in the US, daily reports of Covid-19 deaths have been relatively high for weeks.
There have been more than 455,000 deaths in the US, with 4,805 new deaths reported Thursday, according to data from Johns Hopkins University, though more than 1,500 of the fatalities reported Thursday include backlogged deaths. This is the highest number of deaths the US has reported in a single day since the pandemic began, according to the data.
The country has averaged more than 3,080 Covid-19 deaths a day over the last week – not far from the peak average of 3,357 on January 13, according to Johns Hopkins data. Health experts have said death tallies can be high weeks after cases surge because patients can be sick for weeks.
The United States, meanwhile, could add about 83,000 deaths to the current tally of more than 450,800 by February 27, according to an ensemble forecast by the CDC.
As health experts urge a faster pace for vaccinations to get ahead of more-transmissible variants, the United States may be inching closer to obtaining a third authorized vaccine.
Johnson & Johnson officially asked the US Food and Drug Administration for an emergency use authorization for its one-dose vaccine candidate. If authorized, it would be the third vaccine to be allowed in the US market, joining two-dose products from Pfizer/BioNTech and Moderna.
“Today’s submission for Emergency Use Authorization of our investigational single-shot COVID-19 vaccine is a pivotal step toward reducing the burden of disease for people globally and putting an end to the pandemic,” Dr. Paul Stoffels, chief scientific officer at Johnson & Johnson, said in a statement.
The FDA’s Vaccines and Related Biological Products Advisory Committee will meet February 26 to discuss Johnson & Johnson’s request for emergency use authorization.
Fauci told NBC on Wednesday he would not be surprised if the EUA for Johnson & Johnson “happens within the next week or two.”
Fauci on Thursday tweeted that he hopes there will be data to support Covid-19 vaccinations for older children – between 12 and 17 – by the late spring or summer.
“We will progress to younger age groups as we have more data. This will help reduce virus transmission,” he tweeted from the White House Covid-19 Response Team account during a question and answer session.
CORRECTION: A version of this story on Thursday morning stated that Johnson & Johnson had sought emergency use authorization for its vaccine candidate from the Food and Drug Administration. As of that time, the company had not announced such an application.
CNN’s Andrea Diaz, Ben Tinker, Haley Brink, Naomi Thomas, Kristina Sgueglia, Christopher Rios, John Bonifield, Elizabeth Stuart, Jen Christensen and Deidre McPhillips contributed to this report.